Arthritis Physiotherapy addresses one of the most common causes of long-term joint pain and stiffness in the UK, yet it remains widely misunderstood. Many people still believe arthritis is an unavoidable part of ageing or that movement will worsen symptoms. In reality, both assumptions often lead to poorer outcomes and unnecessary functional decline.
Across clinics, the pattern is familiar. People reduce activity to avoid pain, joints become stiffer, muscles weaken, and everyday tasks gradually feel harder. Arthritis itself has not suddenly worsened — movement confidence and joint support have. Understanding what arthritis actually is, and how it responds to the right kind of treatment, makes a significant difference.
This guide explains how arthritis affects the joints, the most common types seen in the UK, and why Arthritis Physiotherapy remains one of the most effective ways to manage pain, improve mobility, and protect long-term joint health.
What Is Arthritis?
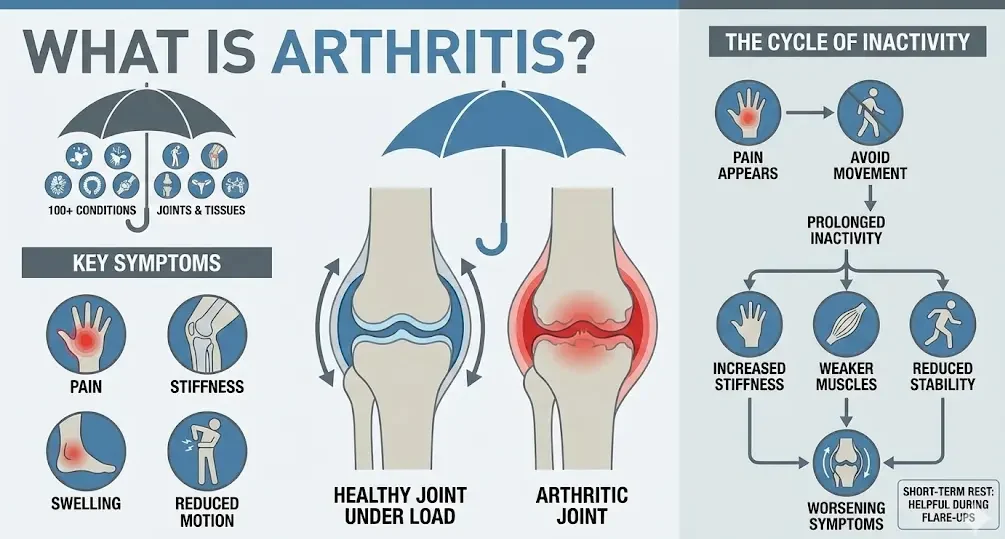
Arthritis is an umbrella term used to describe more than 100 conditions that affect joints and surrounding tissues. While symptoms vary, most forms of arthritis involve pain, stiffness, swelling, and reduced range of motion. These symptoms may develop slowly over time or appear more suddenly, depending on the type of arthritis involved.
Joints are designed to move under load. When pain appears, people often avoid movement to protect the joint. Short-term rest can be helpful during flare-ups, but prolonged inactivity usually leads to increased stiffness, weaker muscles, and reduced joint stability. Over time, this contributes to worsening symptoms rather than relief.
Common Types of Arthritis
1.) Osteoarthritis (OA)
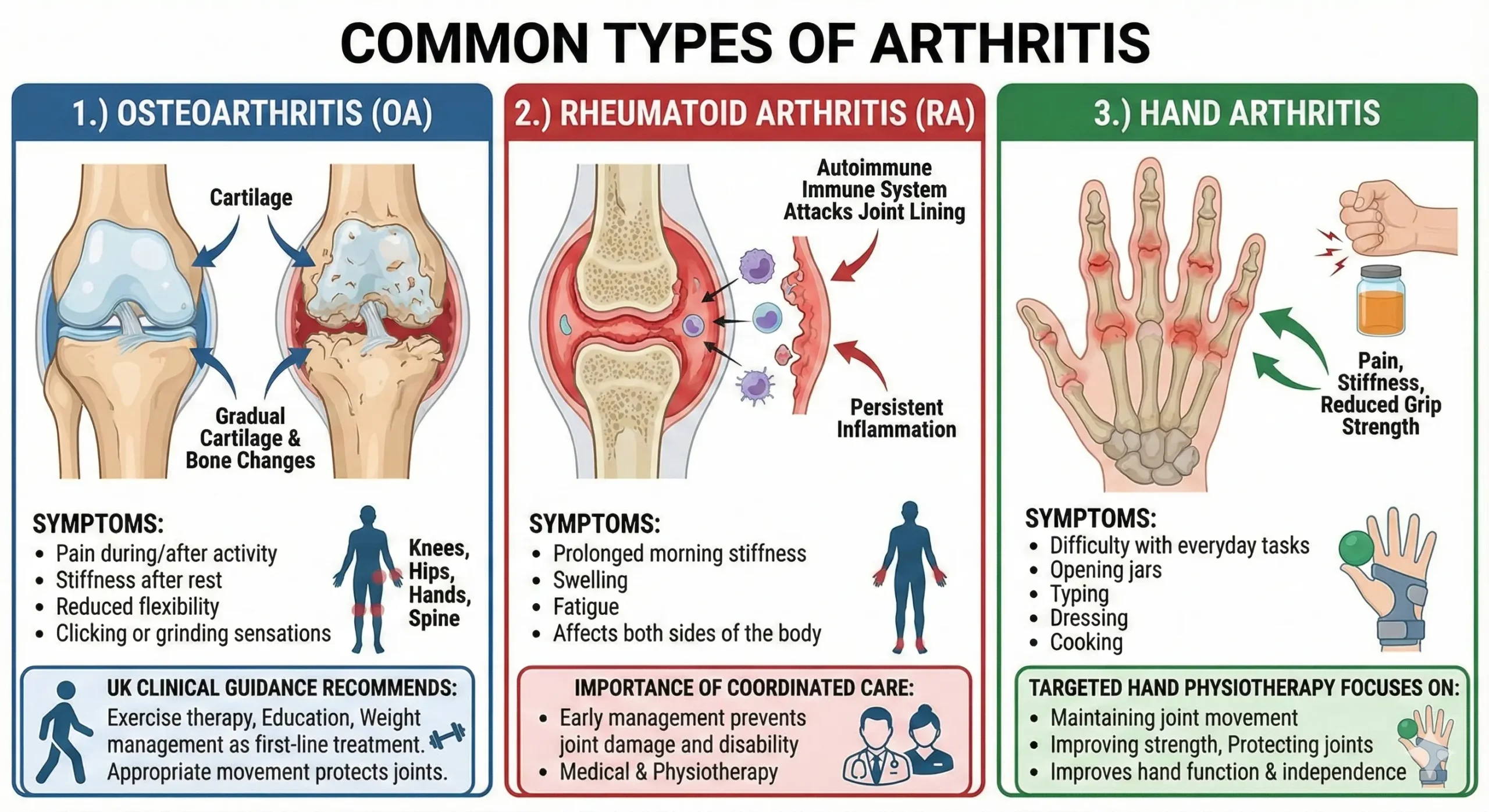
Osteoarthritis is the most common form of arthritis in the UK. It involves gradual changes to cartilage, bone, and surrounding tissues, rather than simple “wear and tear.” These changes affect how the joint moves and tolerates load.
Typical symptoms include pain during or after activity, stiffness after rest, reduced flexibility, and sensations such as clicking or grinding. Knees, hips, hands, and the spine are most frequently affected.
Wendover in UK clinical guidance consistently recommends exercise therapy, education, and weight management as first-line treatment for osteoarthritis. Rest alone does not protect joints—appropriate movement does.
2.) Rheumatoid Arthritis (RA)
Rheumatoid arthritis is an autoimmune condition in which the immune system attacks the joint lining, leading to persistent inflammation. Without early management, this can result in joint damage and long-term disability.
RA often presents with prolonged morning stiffness, swelling, fatigue, and symptoms affecting both sides of the body. Unlike osteoarthritis, rheumatoid arthritis can also affect other systems in the body, which is why coordinated medical and Arthritis Physiotherapy care is important.
3.) Non Rheumatoid Arthritis
‘Non-rheumatoid arthritis’ refers to joint conditions not driven by autoimmune inflammation. Unlike rheumatoid arthritis, the immune system is not attacking the joints. These conditions are usually degenerative, mechanical, metabolic, or injury-related and are far more common in the general population.
Common Types of Non-RA Arthritis
Osteoarthritis (OA)—the most common form. Caused by gradual cartilage wear, joint space narrowing, and bony changes. Frequently affects knees, hips, spine, and hands.
Post-traumatic arthritis – Develops after fractures, ligament injuries, or joint surgery. Damage alters joint mechanics, accelerating degeneration.
Mechanical or overuse arthritis—results from repetitive strain, poor posture, muscle imbalance, or occupational stress (e.g., prolonged desk work, manual labor).
Crystal-induced arthritis—Includes conditions like gout or pseudogout, where crystal deposits trigger acute joint inflammation without autoimmune disease.
Age-related degenerative arthritis—Structural joint changes linked to aging, reduced cartilage resilience, and cumulative load over time.
Key Characteristics
Pain pattern: Typically worsens with activity and improves with rest
Joint involvement: Often asymmetrical and localized
Morning stiffness: Mild and short-lived (usually under 30 minutes)
Systemic symptoms: Absent (no fatigue, fever, or widespread inflammation)
Blood tests: Usually normal; negative for rheumatoid factor (RF) and anti-CCP
Imaging findings: Joint space narrowing, osteophytes, cartilage loss, or post-injury changes rather than erosive inflammatory damage
Management Approach
Non-RA arthritis management focuses on mechanical load control and functional improvement, not immune suppression. This typically includes:
Arthritis Physiotherapy for joint mobility, strength, and movement control
Activity modification and ergonomic correction
Weight management where relevant
Pain management strategies (exercise-based first, medication secondary)
Education to maintain confidence in movement and prevent fear-avoidance
2.) Non-Rheumatoid Arthritis (Non-RA)
Non-Rheumatoid Arthritis refers to joint conditions not driven by autoimmune inflammation. Unlike rheumatoid arthritis, the immune system is not attacking the joints. These conditions are usually degenerative, mechanical, metabolic, or injury-related and are far more common in the general population.
Common Types of Non-RA Arthritis
Osteoarthritis (OA) – The most common form. Caused by gradual cartilage wear, joint space narrowing, and bony changes. Frequently affects knees, hips, spine, and hands.
Post-traumatic arthritis – Develops after fractures, ligament injuries, or joint surgery. Damage alters joint mechanics, accelerating degeneration.
Mechanical or overuse arthritis – Results from repetitive strain, poor posture, muscle imbalance, or occupational stress (e.g., prolonged desk work, manual labor).
Crystal-induced arthritis – Includes conditions like gout or pseudogout, where crystal deposits trigger acute joint inflammation without autoimmune disease.
Age-related degenerative arthritis – Structural joint changes linked to aging, reduced cartilage resilience, and cumulative load over time.
Key Characteristics
Pain pattern: Typically worsens with activity and improves with rest
Joint involvement: Often asymmetrical and localized
Morning stiffness: Mild and short-lived (usually under 30 minutes)
Systemic symptoms: Absent (no fatigue, fever, or widespread inflammation)
Blood tests: Usually normal; negative for rheumatoid factor (RF) and anti-CCP
Imaging findings: Joint space narrowing, osteophytes, cartilage loss, or post-injury changes rather than erosive inflammatory damage
Management Approach
Non-RA arthritis management focuses on mechanical load control and functional improvement, not immune suppression. This typically includes:
Physiotherapy for joint mobility, strength, and movement control
Activity modification and ergonomic correction
Weight management where relevant
Pain management strategies (exercise-based first, medication secondary)
Education to maintain confidence in movement and prevent fear-avoidance
| Arthritis Type | What Patients Commonly Report | Clinical Interpretation | Evidence-Based First Approach |
|---|---|---|---|
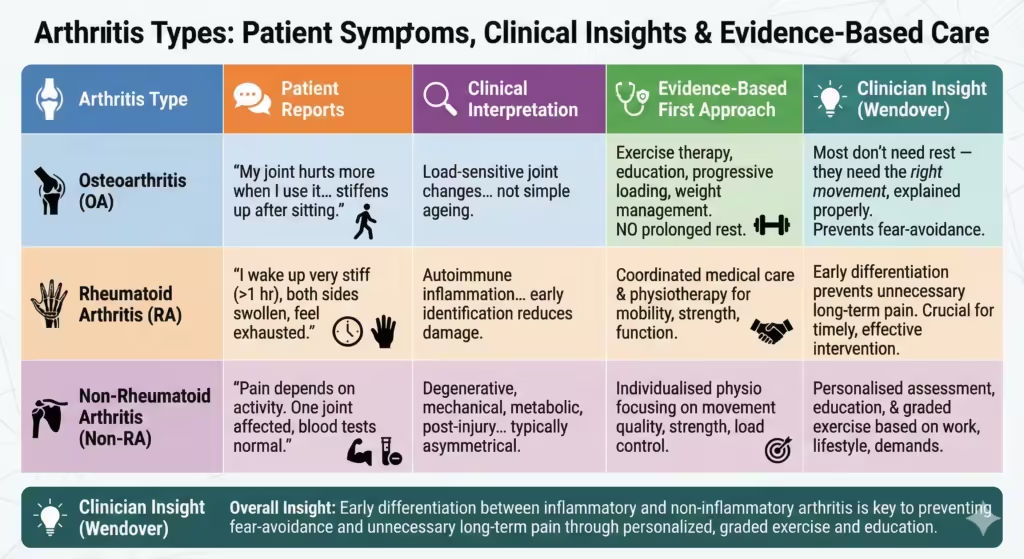
| Osteoarthritis (OA) | “My joint hurts more when I use it, especially after walking or standing. It stiffens up after sitting.” | Load-sensitive joint changes involving cartilage, bone, and surrounding tissues — not simple ageing or inactivity. | Exercise therapy, education, progressive loading, and weight management where appropriate. Prolonged rest is not recommended. |
| Rheumatoid Arthritis (RA) | “I wake up very stiff for over an hour, both sides are swollen, and I feel exhausted.” | Autoimmune inflammation of the joint lining with potential systemic involvement. Early identification reduces long-term joint damage. | Coordinated medical care alongside physiotherapy to maintain joint mobility, strength, and daily function. |
| Non-Rheumatoid Arthritis (Non-RA) | “Pain depends on activity. One joint is affected, blood tests are normal.” | Degenerative, mechanical, metabolic, or post-injury joint conditions without autoimmune disease. Typically localised and asymmetrical. | Individualised physiotherapy focusing on movement quality, strength, load control, and activity confidence. |
| Clinician Insight (Wendover) | “Most arthritis patients we see locally don’t need rest — they need the right movement, explained properly.” | Early differentiation between inflammatory and non-inflammatory arthritis prevents fear-avoidance and unnecessary long-term pain. | Personalised assessment, education, and graded exercise based on work, lifestyle, and joint demands. |
What Causes Arthritis?
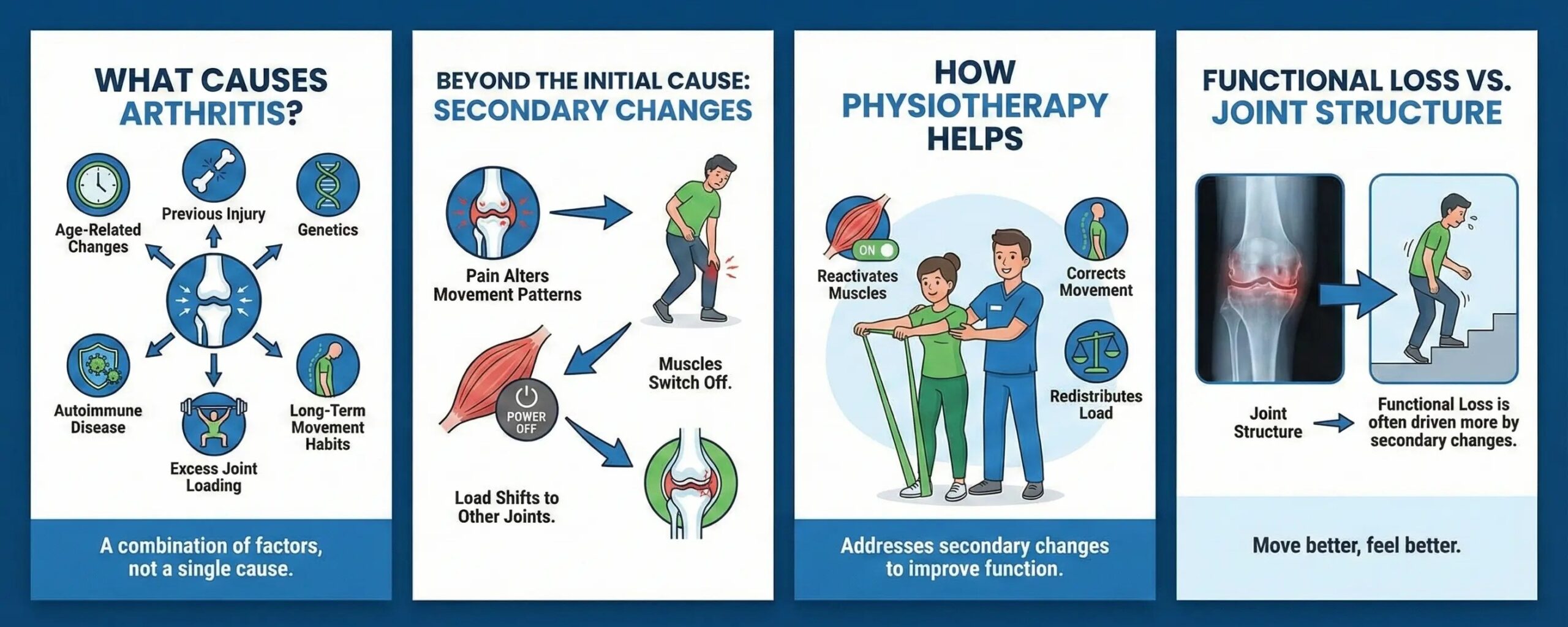
Arthritis rarely has a single cause. It typically develops due to a combination of factors, including age-related joint changes, previous injury, genetics, autoimmune disease, excess joint loading, and long-term movement habits.
What often matters more than the original cause is how joints are managed after symptoms begin. Pain alters movement patterns. Muscles switch off. Load shifts to other joints. Arthritis Physiotherapy addresses these secondary changes, which frequently drive pain and functional loss more than joint structure alone.
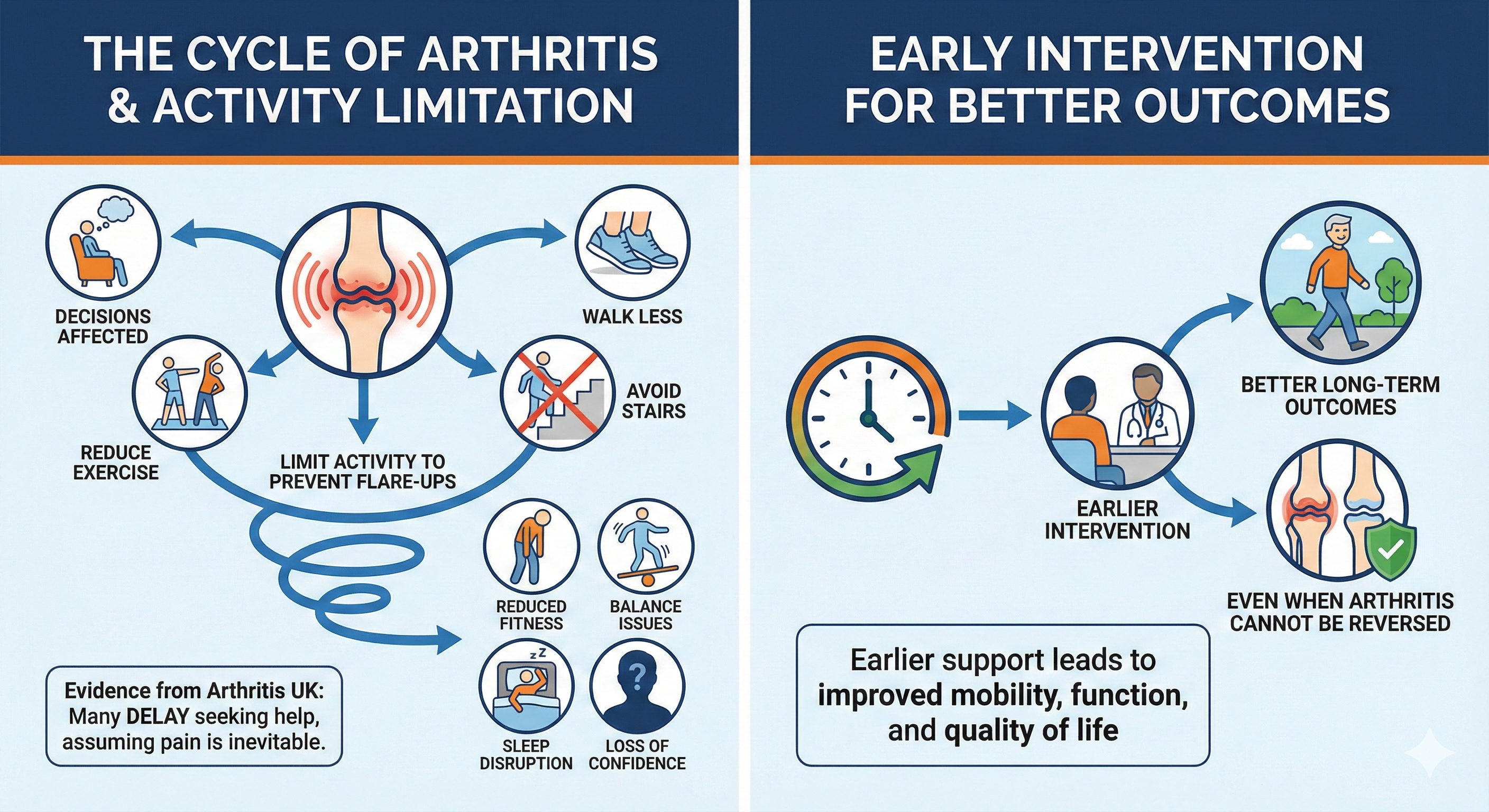
How Arthritis Affects Everyday Life
Arthritis affects more than joints — it affects decisions. People walk less, avoid stairs, reduce exercise, and gradually limit activity to prevent flare-ups. Over time, this leads to reduced fitness, balance issues, sleep disruption, and loss of confidence.
Evidence from Arthritis UK shows that many people delay seeking help, assuming pain is inevitable. In reality, earlier intervention leads to better long-term outcomes, even when arthritis cannot be reversed.

Why Physiotherapy Matters in Arthritis Management
Arthritis Physiotherapy is a core treatment across UK clinical guidance because it targets pain, stiffness, weakness, and loss of function together. Rather than focusing only on joints, physiotherapy looks at how the whole body moves and supports those joints.
Clinical Perspective from Phoenix Physio
In the clinic in Wendover, UK, we regularly see people with arthritis who have been advised to “rest” or avoid movement altogether. In practice, prolonged rest often leads to increased stiffness, weaker muscles, and greater pain sensitivity. Our specialised Arthritis Physiotherapy assess how each joint moves, how it is loaded during daily activity, and how strength, balance, and movement habits contribute to symptoms—not just what scans show.
Physiotherapy for Different Types of Arthritis
1.) Osteoarthritis Physiotherapy
For osteoarthritis, physiotherapy focuses on improving muscle strength, joint stability, and movement control. Stronger muscles reduce joint stress, while better movement patterns improve load tolerance. Education around pacing and activity modification helps people stay active without fear.
Research consistently shows that exercise-based treatment reduces pain and improves function in osteoarthritis, often achieving benefits that match or exceed those of medication.
2.) Rheumatoid Arthritis Physiotherapy
In rheumatoid arthritis, physiotherapy adapts to disease activity. During flare-ups, the focus is gentle movement and stiffness management. During stable phases, strengthening and aerobic exercise help maintain physical capacity and overall health.
This flexible approach allows people to remain active without aggravating inflamed joints.
3.) Non-Rheumatoid Arthritis Physiotherapy (Non-RA)
Non-rheumatoid arthritis physiotherapy focuses on mechanical joint health, not immune suppression. Because Non-RA conditions are not driven by autoimmune inflammation, treatment is built around improving movement quality, joint tolerance, strength, and daily function, rather than rest or passive care.
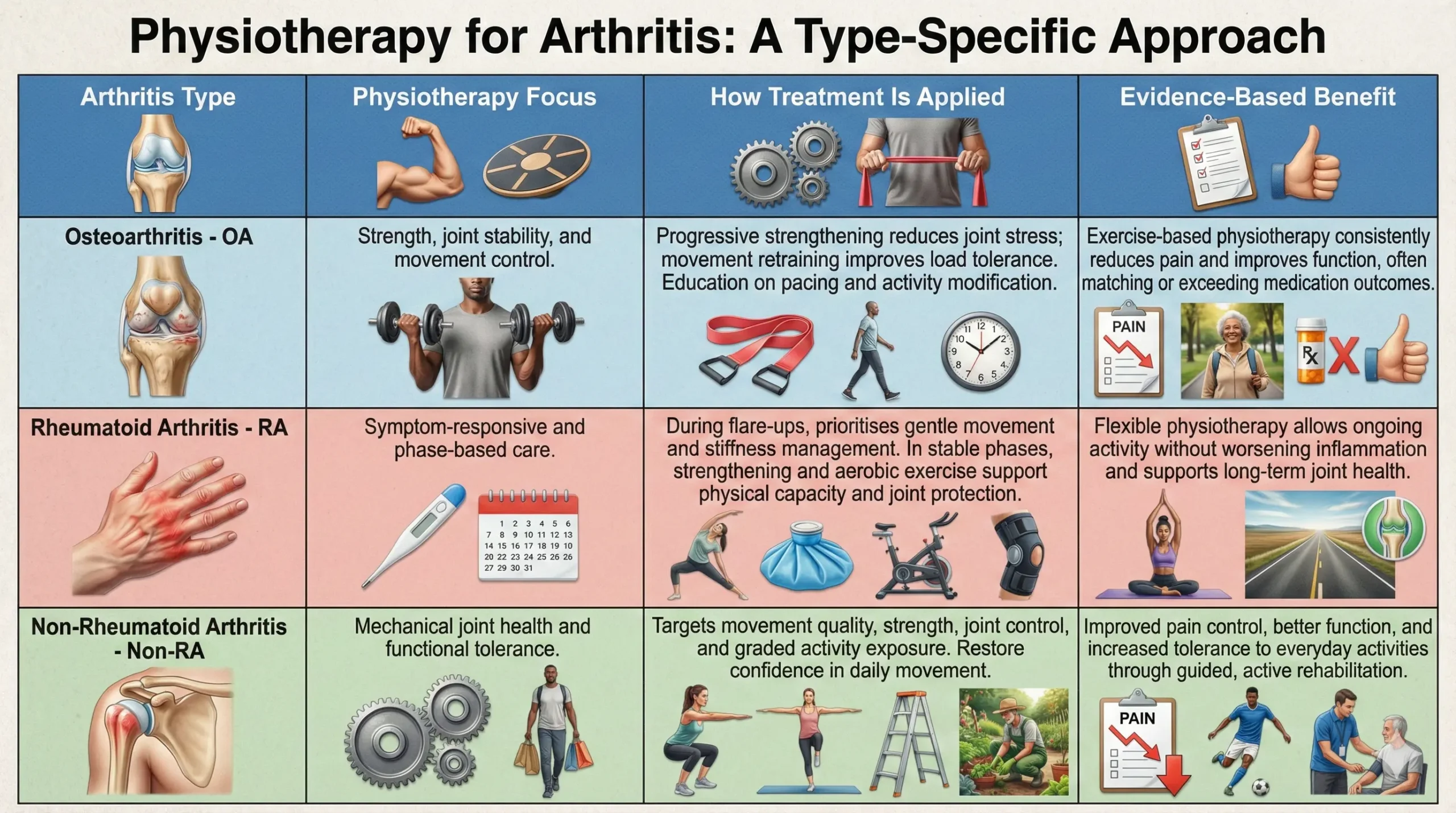
| Arthritis Type | Physiotherapy Focus | How Treatment Is Applied | Evidence-Based Benefit |
|---|---|---|---|
| Osteoarthritis (OA) | Strength, joint stability, and movement control | Progressive strengthening reduces joint stress, while movement retraining improves load tolerance. Education on pacing and activity modification helps people stay active without fear of damage. | Exercise-based physiotherapy consistently reduces pain and improves function, often matching or exceeding medication outcomes. |
| Rheumatoid Arthritis (RA) | Symptom-responsive and phase-based care | During flare-ups, physiotherapy prioritises gentle movement and stiffness management. In stable phases, strengthening and aerobic exercise support physical capacity and joint protection. | Flexible physiotherapy allows ongoing activity without worsening inflammation and supports long-term joint health. |
| Non-Rheumatoid Arthritis (Non-RA) | Mechanical joint health and functional tolerance | Treatment targets movement quality, strength, joint control, and graded activity exposure. Focus is on restoring confidence in daily movement rather than rest or passive treatment. | Improved pain control, better function, and increased tolerance to everyday activities through guided, active rehabilitation. |

The Role of Exercise in Arthritis
Exercise is one of the most effective tools for managing arthritis symptoms and protecting joint health. When done correctly, exercise improves strength, movement control, and pain regulation without damaging joints. Regular activity helps joints tolerate load and reduces stiffness and sensitivity over time.
Different forms of exercise serve different purposes. Strength training supports and offloads joints, aerobic exercise improves general health and pain control, mobility work reduces stiffness, and balance training lowers fall risk. Together, these forms of exercise support safer, more confident movement.
There is no single exercise programme that suits everyone with arthritis. Exercise must be tailored to symptoms, affected joints, and daily demands. Physiotherapy guidance ensures exercise is appropriate, progressive, and effective for long-term symptom control.

Lifestyle Factors That Influence Arthritis Symptoms
Lifestyle choices strongly influence how arthritis behaves, often more than people expect. Daily habits such as physical activity levels, body weight, sleep quality, and stress directly affect pain sensitivity, joint loading, and how well joints tolerate movement. Periods of inactivity, poor sleep, or ongoing stress can increase stiffness and pain even when joint structure has not changed.
Key lifestyle factors that influence arthritis symptoms include:
Physical activity levels – Regular movement maintains joint mobility, muscle strength, and confidence in activity.
Body weight management – Excess weight increases mechanical load on joints such as the knees, hips, and spine.
Sleep quality – Poor sleep heightens pain sensitivity and slows tissue recovery.
Stress levels – Ongoing stress can amplify pain signals and trigger symptom flare-ups.
Recovery habits – Adequate rest between activity supports joint tolerance and long-term function.
While diet alone does not cure arthritis, consistent movement and supportive recovery habits play a central role in symptom control. Balanced nutrition supports tissue health, structured exercise improves joint resilience, and stress management helps stabilise pain levels. When combined, these lifestyle choices support better day-to-day comfort, improved function, and long-term joint health for people living with arthritis.

When Should You See a Physiotherapist?
You should see an Arthritis Physiotherapy as soon as joint pain, stiffness, or loss of movement starts to change how you move or what you avoid doing. Symptoms do not need to be severe. Mild but persistent pain is often the earliest sign that joints are no longer being supported properly.
Many people wait until pain is constant or mobility is clearly reduced. By then, muscles are weaker, joints are less stable, and movement patterns have adapted around pain. Physiotherapy can still help at this stage, but recovery is slower, and flare-ups are more likely.
Arthritis physiotherapy is especially important if you notice morning stiffness, pain during or after activity, or difficulty walking, climbing stairs, or gripping objects, or if you reduce activity to avoid discomfort. These changes usually worsen without targeted intervention.
Early Arthritis Physiotherapy focuses on improving joint control, restoring strength, and normalizing movement. This reduces flare-ups, limits functional decline, and helps people stay active and independent for longer. Waiting until symptoms become severe often narrows treatment options and prolongs recovery.
How Does Phoenix Physio Help People With Arthritis Physiotherapy?
At Phoenix Physio in Wendover, UK, Arthritis Physiotherapy begins with a detailed understanding of how your joints move, how your muscles support those joints, and how arthritis symptoms affect your daily activities. Rather than treating pain in isolation, the assessment looks at movement quality, joint loading, strength, flexibility, and confidence in movement.
Arthritis Physiotherapy treatment is individual and evidence-based, recognising that no two people experience arthritis in the same way. Programmes are tailored to the type of arthritis, the joints involved, and your lifestyle demands, whether that includes work, exercise, or everyday tasks. Treatment progresses gradually to improve joint tolerance, reduce pain sensitivity, and restore functional movement without unnecessary strain.
The focus of Arthritis Physiotherapy at Phoenix Physio is long-term joint health, not short-term relief alone. Through guided exercise, education, and activity planning, patients are supported to stay active, move confidently, and manage symptoms sustainably. This approach helps build stronger joints, better movement control, and lasting improvements in daily function over time.
If joint pain is limiting your movement, now is the right time to take control. Booking an appointment for Arthritis Physiotherapy in Wendover, UK at Phoenix Physio gives you a clear, structured plan built around your joints, your lifestyle, and your goals. Early assessment helps prevent stiffness from progressing, improves joint strength, and restores confidence in daily activities before symptoms become harder to manage.

Conclusion
Arthritis does not mean giving up movement or accepting ongoing pain. Arthritis Physiotherapy focuses on restoring joint control, improving strength, and reducing unnecessary stress on affected joints. With the right Arthritis Physiotherapy approach, people can reduce symptoms, improve mobility, and stay active for far longer than expected. Early, informed Arthritis Physiotherapy plays a key role in protecting joint health, function, and long-term quality of life.
Frequently Asked Questions (FAQs)
Can physiotherapy really help arthritis?
Yes. Arthritis Physiotherapy is strongly supported by Phoenix Physio UK clinical guidance. It reduces pain, improves strength and mobility, and helps protect joints. Exercise-based physiotherapy is one of the most effective non-surgical treatments for arthritis.
Is exercise & Arthritis Physiotherapy safe if I have arthritis?
Yes, when guided correctly. Appropriate exercise strengthens joints and reduces stiffness. Avoiding movement often leads to worse pain, reduced function, and faster physical decline.
When should I start Arthritis Physiotherapy for arthritis?
As early as possible. Early Arthritis Physiotherapy improves movement quality, slows functional decline, and reduces long-term pain. You do not need severe symptoms to benefit.
Do I need surgery for arthritis?
Most people do not. Conservative management, including physiotherapy and education, is effective for many. Surgery is usually considered only when non-surgical options no longer help.
Can arthritis be cured?
Arthritis Physiotherapy cannot cure most types of arthritis, but it plays a key role in managing symptoms effectively. Targeted physiotherapy helps reduce pain, maintain movement, and support long-term independence and activity levels.
Can I live a long life with arthritis?
Inflammatory arthritis is a condition many people endure for a lifetime. Thanks to advances in treatment, however, innovative medications can delay and even halt the progression of the disease, and non-drug approaches have can help relieve symptoms so you can live a full and productive life.
What is the best treatment for arthritis in the neck?
Physical therapy.
Specific exercises can help relieve pain, as well as strengthen and stretch weakened or strained muscles. In some cases, physical therapy may include posture therapy or the use of traction to gently stretch the joints and muscles of your neck.


