Introduction
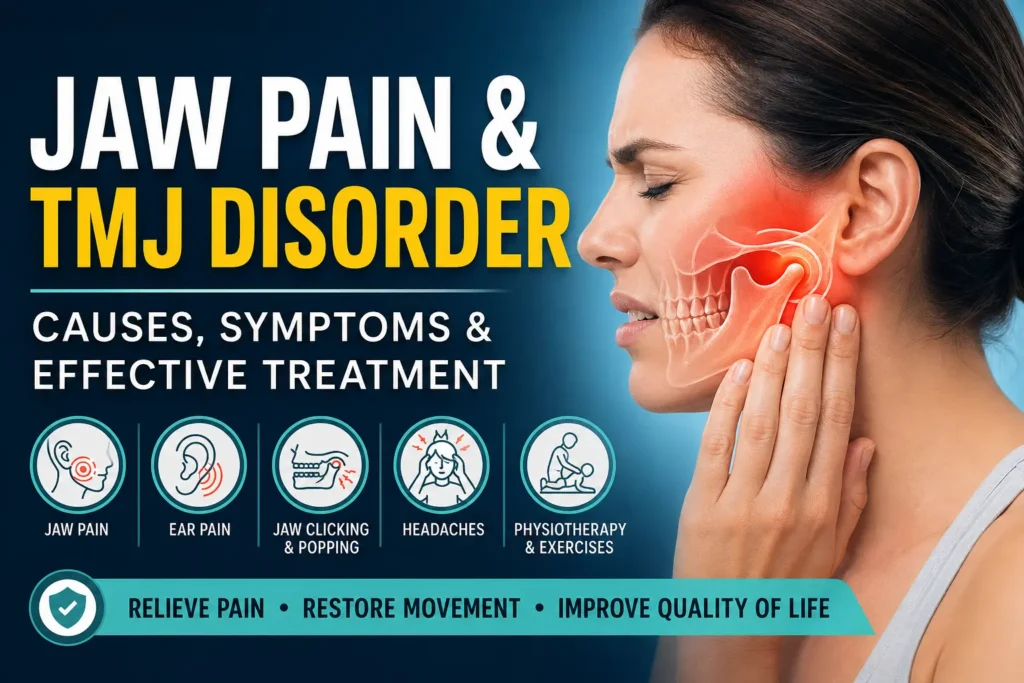
Jaw pain, clicking, or a tight jaw when you wake up are more common than most people realize—and often misunderstood. Whether it’s jaw pain on one side, pain under the ear behind the jaw bone, or a clicking jaw when chewing, these symptoms usually point to a problem with the temporomandibular joint (TMJ) or surrounding muscles.
Temporomandibular disorder (TMD) doesn’t just affect your jaw. It can trigger headaches, ear pain, neck stiffness, and even dizziness—which is why many people treat the wrong area for months without getting real relief.
This guide breaks down what your jaw pain actually means, the most common causes of TMD, how to relieve symptoms safely at home, and when to seek physiotherapy. If your jaw keeps clicking, locking, or aching, understanding the cause is the first step to fixing it properly.
That Jaw Ache Pain — What Does It Actually Mean?
A dull jaw ache is something a lot of people push through for months before seeking help. It might start as jaw discomfort on one side when you wake up, then gradually become a near-constant companion—a tight, tired feeling that spreads from the joint up towards your temple or down towards your neck.
The most common reason? The temporomandibular joint — the hinge that connects your lower jaw to your skull — is under strain. This can be from muscle overuse (think: clenching your teeth at night, chewing on one side, or carrying tension in your jaw during stressful periods), from disc displacement within the joint, or from changes in how the upper and lower teeth meet.
One-Sided vs. Both Sides: Does It Matter?
If your jaw hurts on the left side specifically — or you notice jaw pain in the left side of your face — this often points to an imbalance. Maybe you sleep on your left side, favour that side when chewing, or the left TMJ disc has shifted. The same applies on the right. One-sided jaw discomfort usually means one joint or one muscle group is working harder than the other.
When jaw pain affects both sides simultaneously, the cause tends to be systemic muscle tension — widespread clenching or bruxism (grinding) that loads both joints equally. Both presentations respond well to physiotherapy, though the approach differs slightly.
| Where It Hurts | Common Pattern | What It Often Suggests |
|---|---|---|
| Jaw hurts on left side / right side only | Pain when chewing, yawning, or waking up | Unilateral TMJ dysfunction, disc issue, or muscle imbalance |
| Pain under ear behind jaw bone | Deep ache, sometimes throbbing | TMJ joint inflammation, capsule irritation, or referred ear pain |
| Jaw discomfort on both sides | Fatigue, tightness, morning stiffness | Teeth grinding (bruxism) or widespread muscle tension |
| Jaw pain in left side of face spreading to temple | Headache, pressure, ear fullness | Temporalis muscle referral pain or TMJ disorder (TMD) |

Clicking Jaw, Popping & Temporomandibular Disorder (TMD)
A clicking jaw is one of the most Googled jaw complaints—and for good reason. That snap, crackle, or pop when you open wide, yawn, or chew is hard to ignore once you notice it. The technical name is TMJ clicking, and it’s one of the hallmark signs of temporomandibular disorder (TMD).
It happens when the small fibrocartilage disc inside the joint slips slightly out of position and then “pops” back as the mouth opens or closes. The click itself isn’t always painful—but it can become painful, and it often comes with other symptoms that make life a bit miserable: jaw stiffness in the mornings, restricted mouth opening, and difficulty finishing a meal.
Why Does My Jaw Click When I Chew — or Just in the Morning?
Jaw clicking on one side during eating typically means the disc on that side has a degree of anterior displacement. Clicking specifically in the morning can reflect overnight clenching that loads the joint and shifts the disc while you sleep. If the clicking is present only on wide openings and not painful, it may be managed conservatively. If it’s getting louder, more frequent, or associated with locking—that’s the time to get it properly assessed.
What Is a TMD Therapist, and Do You Need One?
A TMD therapist is typically a physiotherapist with additional training in craniofacial and jaw conditions. They assess how the joint moves, screen the surrounding musculature, check for referral patterns into the neck and head, and develop a plan that might include manual therapy, specific exercises for temporomandibular joint dysfunction, postural work, and advice on habits that load the joint (like chewing gum, biting nails, or resting with your chin on your hand).
At Phoenix Physiotherapy Aylesbury, our team is experienced in assessing and managing TMD — including cases where patients have already seen multiple practitioners without getting clear answers.
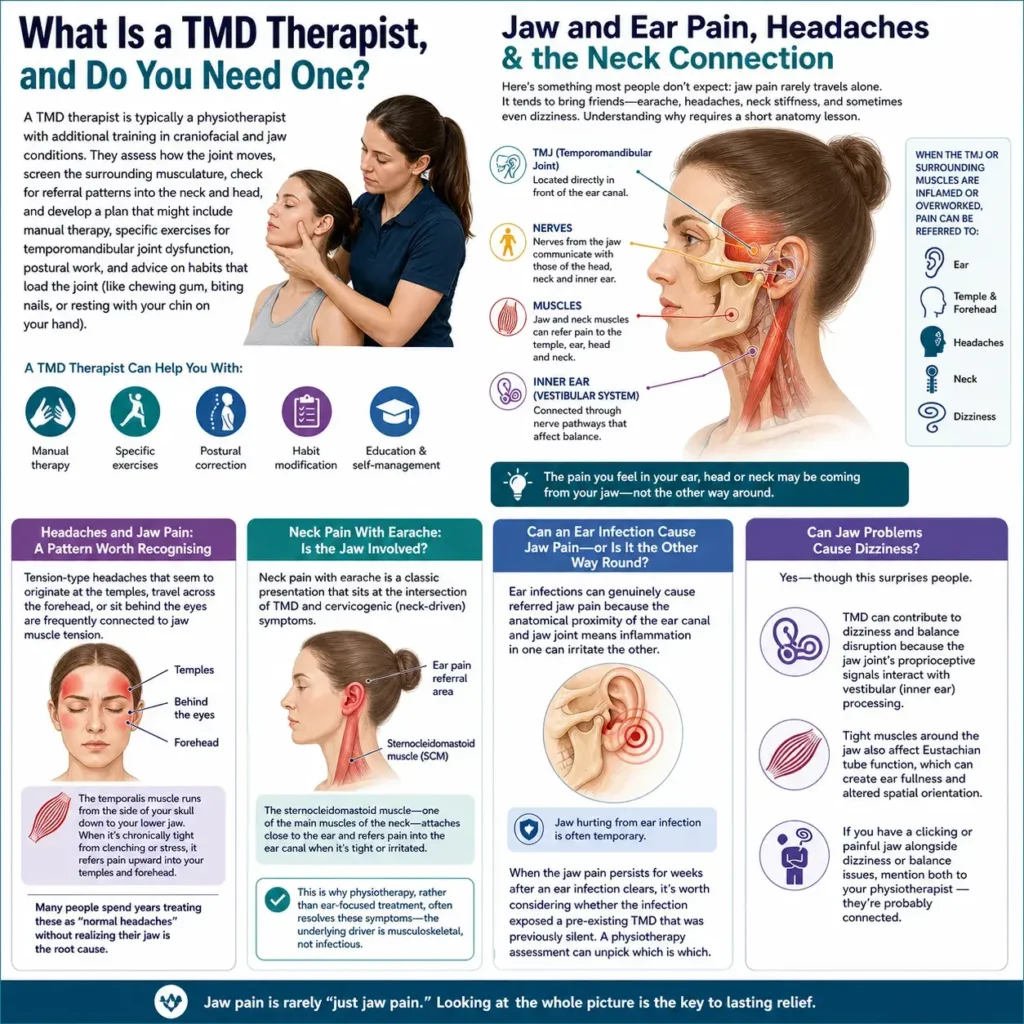
Jaw and Ear Pain, Headaches & the Neck Connection
Here’s something most people don’t expect: jaw pain rarely travels alone. It tends to bring friends—earache, headaches, neck stiffness, and sometimes even dizziness— Understanding why requires a short anatomy lesson.
The temporomandibular joint sits directly in front of the ear canal. The nerves and muscles that serve the jaw also communicate with those of the neck, skull, and inner ear. So when the TMJ or its surrounding muscles are inflamed or overworked, pain can be referred almost anywhere in this region.
Headaches and Jaw Pain: A Pattern Worth Recognising
Tension-type headaches that seem to originate at the temples, travel across the forehead, or sit behind the eyes are frequently connected to jaw muscle tension. The temporalis muscle runs from the side of your skull down to your lower jaw — when it’s chronically tight from clenching or stress, it refers pain upward into your temples and forehead. Many people spend years treating these as “normal headaches” without realizing their jaw is the root cause.
Neck Pain With Earache: Is the Jaw Involved?
Neck pain with earache is another classic presentation that sits at the intersection of TMD and cervicogenic (neck-driven) symptoms. The sternocleidomastoid muscle—one of the main muscles of the neck—attaches close to the ear and refers pain into the ear canal when it’s tight or irritated. So the complaint of “my ear and jaw hurt on the same side” might actually originate from the neck rather than the ear itself.
This also explains why physiotherapy, rather than an ear-focused treatment, often resolves these symptoms—the underlying driver is musculoskeletal, not infectious.
Can an Ear Infection Cause Jaw Pain—or Is It the Other Way Round?
Ear infections can genuinely cause referred jaw pain because the anatomical proximity of the ear canal and jaw joint means inflammation in one can irritate the other. That said, jaw hurting from ear infection is often temporary. When the jaw pain persists for weeks after an ear infection clears, it’s worth considering whether the infection exposed a pre-existing TMD that was previously silent. A physiotherapy assessment can unpick which is which.
Can Jaw Problems Cause Dizziness?
Yes — though this surprises people. TMD can contribute to dizziness and balance disruption because the jaw joint’s proprioceptive signals interact with vestibular (inner ear) processing. Tight muscles around the jaw also affect Eustachian tube function, which can create a sense of ear fullness and altered spatial orientation. If you have a clicking or painful jaw alongside dizziness or balance issues, mention both to your physiotherapist—they’re probably connected.
When Does Your Jaw Pain Flare Up? Identifying Your Triggers
The timing of jaw pain is one of the most useful pieces of information for diagnosis. Below are the patterns we hear most often at Phoenix Physio — and what they tend to indicate.
Jaw Pain After Eating
Pain during or after meals suggests the muscles of mastication (chewing muscles — masseter, temporalis, medial pterygoid) are fatiguing under load. If hard foods or long meals consistently worsen your jaw ache, this is a reliable sign that the muscles and/or joint are under mechanical stress. Temporarily sticking to softer foods is a sensible short-term measure, but it doesn’t address the underlying cause.
Jaw Pain After Yawning — and Neck Pain While Yawning
A painful wide yawn is almost textbook TMD. The joint has to open to its maximum range during a yawn, and if the disc is displaced or the joint capsule is inflamed, this stretch provokes pain. Neck pain while yawning, alongside jaw discomfort, is also common—the deep neck flexors and suboccipital muscles work together with the jaw muscles during wide mouth opening, so strain in one region compounds the other.
Jaw Pain at Night and After Sleep
Waking up with jaw discomfort — a tight, stiff, achy jaw after sleep — almost always points to nocturnal bruxism (teeth clenching or grinding during sleep). You might not know you’re doing it; many people are completely unaware until a partner mentions it or a dentist notices the wear pattern on their teeth. Physiotherapy won’t replace a night guard if grinding is severe, but it addresses the muscular tension that drives the habit.
Crunching in the Ear When Moving the Jaw
A crunching, crackling, or grinding sensation in the ear when moving the jaw — rather than a clean click — is called crepitus. It typically reflects degenerative changes within the joint surface, or adhesions within the joint space. It’s less common than simple clicking, tends to occur in older individuals or those with a long history of untreated TMD, and benefits from a different therapeutic approach. It isn’t always painful, but it’s a signal that the joint has been under prolonged stress.

Exercises for Temporomandibular Joint Dysfunction — What Actually Works
Exercise is one of the most evidence-backed treatments for TMD — but only when it’s the right exercise, done correctly. Generic jaw-stretching advice from the internet is a starting point, not a treatment plan. Here’s a brief overview of exercises commonly used in physiotherapy for temporomandibular joint syndrome, along with what they’re targeting.
The “Chin Tuck and Jaw Rest” Position
What it does: Reduces the compressive load on the TMJ and retrains the resting jaw position. Many people unknowingly press their tongue to the roof of the mouth while holding their teeth together, which increases joint compression over time.
How: Gently tuck your chin in (like making a “double chin”), keep teeth slightly apart, lips softly closed, tongue resting lightly on the palate just behind the upper front teeth. Hold for 30 seconds and repeat throughout the day.
Resisted Mouth-Opening Exercise
What it does: Strengthens the suprahyoid muscles and helps recapture a displaced disc over time. This is one of the most clinically studied exercises for temporomandibular joint dysfunction.
How: Place your thumb under your chin, apply gentle upward pressure, and slowly open your mouth against that resistance. Open as wide as comfortable, hold briefly, and close. Repeat 10 times, twice daily. Your physiotherapist will advise on the resistance level.
Lateral Deviation Exercises
What it does: Improves symmetrical jaw movement and reduces muscle imbalance between the two sides—particularly useful if your jaw deviates to one side as you open wide.
How: Slowly move the lower jaw to the left, hold for 3 seconds, and return to the centre. Then to the right. Repeat 10 times on each side. Use a mirror to watch for deviation and correct it.
TMJ Massage — Is It Safe to Do at Home?
TMJ massage — specifically self-massage of the masseter, temporalis, and pterygoid muscles — can bring meaningful short-term relief from jaw tightness. The masseter is the thick muscle on the side of your jaw (feel it clench when you bite down). Gentle circular pressure into it, working upward to the cheekbone and downward toward the jawline, can reduce muscle-driven jaw ache within minutes.
The medial pterygoid (the mirror muscle on the inside of the jaw) is harder to access and is best addressed by a physiotherapist using intraoral massage techniques—don’t attempt this yourself. Temporalis massage along the temple is safe and straightforward — use the pads of your fingers in small circles across the temporal region.
How to Stop Jaw Pain Immediately — First-Line Self-Care
When your jawache flares acutely, the following measures can help within the same day:
- Warm compress: 15–20 minutes of gentle heat over the jaw reduces muscle spasm quickly. A warm (not hot) flannel works fine.
- Soft diet: Give the joint a rest — avoid crusty bread, raw carrots, chewing gum, and anything that requires extended chewing.
- Teeth-apart position: Consciously keep teeth apart with lips closed throughout the day. Every time your teeth rest together (not during eating), you are subtly loading the joint.
- Neck and shoulder release: Jaw tension and neck tension are closely linked. Gentle neck stretches and shoulder rolls can reduce the overall load.
- Avoid wide opening: Skip yawning as wide as possible, and avoid dental appointments that require prolonged wide opening while the joint is flared—ask your dentist for frequent breaks.
These measures are useful stopgaps, but they don’t address disc position, muscle imbalance, or contributing postural patterns. If your jaw pain is recurrent or has lasted more than a few weeks, a physiotherapy assessment at our Aylesbury clinic is the most effective next step.
When Jaw Pain Is Something More Serious — Red Flags to Know
The overwhelming majority of jaw pain is musculoskeletal—TMD, muscle tension, bruxism—and is safely managed with physiotherapy. However, there are a few situations where jaw pain requires urgent medical attention rather than physiotherapy:
- Jaw pain and chest pain or left arm pain: These can be symptoms of a cardiac event. If jaw pain comes on suddenly alongside chest tightness, shortness of breath, or pain radiating down the left arm, call 999 immediately. This is a medical emergency, not a physiotherapy case.
- Jaw that locks completely open or closed: Acute TMJ dislocation requires same-day medical assessment, not exercises.
- Jaw pain after a direct impact or trauma: Rule out fracture with imaging before beginning any treatment.
- Rapidly progressive difficulty swallowing or opening the mouth: This should be evaluated medically to exclude infection (Ludwig’s angina or dental abscess spreading into surrounding tissues).
If none of these apply and your jaw pain has been building gradually, fluctuates with stress or food choices, or comes with clicking, you’re almost certainly looking at a musculoskeletal problem that physiotherapy can genuinely help with.
| Self-Care Method | What to Do | Why It Helps |
|---|---|---|
| Warm Compress | Apply gentle heat for 15–20 minutes using a warm (not hot) flannel | Relaxes tight jaw muscles and reduces spasm quickly |
| Soft Diet | Avoid hard, chewy foods like crusty bread, raw carrots, and chewing gum | Reduces strain on the temporomandibular joint and allows it to settle |
| Teeth-Apart Position | Keep teeth slightly apart with lips closed (except when eating) | Prevents constant joint loading and reduces unnecessary pressure |
| Neck & Shoulder Release | Perform gentle neck stretches and shoulder rolls | Reduces linked tension that often contributes to jaw pain |
| Avoid Wide Opening | Limit wide yawning and request breaks during dental visits | Prevents overstressing an already irritated joint |
Jaw Pain Physiotherapy near Aylesbury — Why Phoenix Physio?
The Phoenix Physio Aylesbury clinic treats jaw pain and TMD regularly. People come from across the Aylesbury Vale—from Buckingham, Wendover, Thame, and surrounding villages—many of whom have been told “it’ll settle on its own” or sent for investigations that come back clear, leaving them no closer to an answer.
Our approach to jaw pain is thorough: we assess the joint itself, the surrounding musculature, the neck and upper thoracic spine (which are almost always involved), bite and jaw movement patterns, and contributing postural and lifestyle factors. Treatment typically combines hands-on physiotherapy, tailored exercises for temporomandibular joint dysfunction, and clear self-management guidance—so patients leave each session knowing exactly what they can do to support recovery between appointments.
We also work closely with dentists and GPs in the Aylesbury area, and can communicate directly with your team if a mouthguard, dental splint, or other co-management is appropriate alongside physiotherapy.
Conclusion
Jaw pain, clicking, and stiffness are some of the most common signs of temporomandibular disorder (TMD). Whether it’s jaw pain on one side, pain under the ear behind the jawbone, or a clicking jaw when chewing, these symptoms are usually linked to muscle tension, joint dysfunction, or habits like clenching and grinding.
While short-term relief strategies like heat, soft diet, and jaw exercises can help, they don’t fix the underlying issue. Persistent jaw ache, headaches linked to jaw tension, or ear pain with jaw movement often require a structured, evidence-based approach to fully resolve.
Physiotherapy plays a key role in treating TMD by addressing the root cause — improving jaw mechanics, reducing muscle overload, and correcting contributing factors from the neck and posture. With the right treatment plan, most people see significant improvement without the need for medication or invasive procedures.
Bottom line: if your jaw pain, clicking, or tightness keeps returning, don’t ignore it. Early assessment and targeted physiotherapy treatment can stop the cycle, restore normal jaw function, and prevent long-term joint problems.